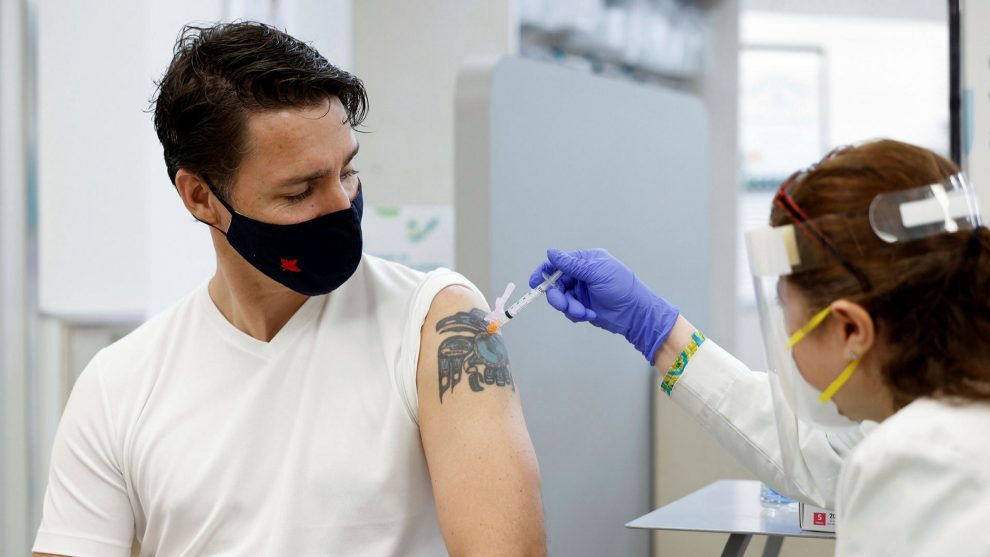
A team of researchers from the University of Gothenburg has just taken another step toward understanding how the immune system develops resistance against COVID-19.
For six months, the researchers at the University’s Sahlgrenska Academy investigated 156 employees from five primary care health facilities who were recruited during April and May 2020. None of these employees had been vaccinated against COVID-19, and the majority of them had to work with infected patients on a daily basis during the height of the pandemic.
They identified IgA (immunoglobulin A) in the respiratory tracts of several of the personnel who didn’t catch COVID-19, which could mean they had an antidote in their immune systems all this time.
These antibodies are found naturally in mucous membrane secretions in the airways and gastrointestinal tract, where they protect the body by binding to viruses and other invading organisms.
An antidote in the immune system
COVID-19, an infectious disease caused by the SARS-CoV-2 virus, has claimed the lives of more than 6 million people since the start of the pandemic in early 2020. In fact, some researchers say the true number of lives lost to the COVID-19 by 31 December 2021 was 18.2 million, which is more than three times the official death toll.
The disease appears to affect some people more severely than others, with some experiencing very minor symptoms and others being hospitalized and requiring aid in breathing. The current study aimed to uncover health factors that appeared to offer COVID-19 protection for the unvaccinated.
“We all have IgA,” said Christine Wennerås, Professor of Clinical Bacteriology at Sahlgrenska Academy, University of Gothenburg, and senior physician at Sahlgrenska University Hospital, who is part of the research team. “It’s found on the mucous membranes, and COVID-19 is an infection that spreads via those membranes. We thought it was important to investigate what happened when completely healthy people encountered the coronavirus, before vaccines became available.”
“Of the participants in our study, none whom contracted COVID-19 required hospitalization,” she continued. “A lot of other research has concerned the most seriously ill patients, who have been hospitalized and in need of intensive care.”
Health factors
According to the results of the study published in the European Journal of Immunology, a third of the care workers developed antibodies to COVID-19, and they fell into two distinct groups based on antibody patterns and COVID-19 incidence.
One group that exclusively possessed IgA antibodies never succumbed to COVID-19. Participants in the other group had IgG antibodies as well as T cells and got the sickness.
The participants who did not test positive or were unwell all had IgA antibodies. Other characteristics that seemed to provide protection against infection were being female and having a respiratory allergy.
The data, however, does not support the notion that those who do not have antibodies against COVID-19 have protective T cells, which are a part of the immune system that focuses on specific foreign particles.
It should be noted that the majority of the COVID-19 vaccines are highly effective against severe illness, hospitalization, and death. In fact, as the Omicron subvariant BA.2 replaces its sister version, BA.1, as the dominant form of COVID-19 in many countries, researchers have discovered that two doses of COVID vaccination still appear to reduce the risk of infection caused by the new subvariant.
Study Abstract:
The patterns of humoral and cellular responses to SARS-CoV-2 were studied in Swedish primary health care workers (n = 156) for 6 months during the Covid-19 pandemic. Serum IgA and IgG to SARS-CoV-2, T-cell proliferation and cytokine secretion, demographic and clinical data, PCR-verified infection, and self-reported symptoms were monitored. The multivariate method OPLS-DA was used to identify immune response patterns coupled to protection from Covid-19. Contracting Covid-19 was associated with SARS-CoV-2-specific neutralizing serum IgG, T cell, IFN-γ, and granzyme B responses to SARS-CoV-2, self-reported typical Covid-19 symptoms, male sex, higher BMI, and hypertension. Not contracting Covid-19 was associated with female sex, IgA-dominated, or no antibody responses to SARS-CoV-2, airborne allergy, and smoking. The IgG-responders had SARS-CoV-2-specific T-cell responses including a cytotoxic CD4+ T-cell population expressing CD25, CD38, CD69, CD194, CD279, CTLA-4, and granzyme B. IgA-responders with no IgG response to SARS-CoV-2 constituted 10% of the study population. The IgA responses were partially neutralizing and only seen in individuals who did not succumb to Covid-19. To conclude, serum IgG-dominated responses correlated with T-cell responses to SARS-CoV-2 and PCR-confirmed Covid-19, whereas IgA-dominated responses correlated with not contracting the infection.
Story cited here.